What Are the Problems With All-on-4 Dental Implants? Risks and Reality
All-on-4 dental implants are one of the most talked-about tooth replacement options available today. The idea of getting a full set of fixed teeth using just four implants sounds like a simple solution to a complex problem. And for many patients, it truly is life-changing.
But like any surgical procedure, All-on-4 comes with real risks. If you are considering this treatment, you deserve an honest look at what can go wrong, why it happens, and how to protect yourself from costly complications.
What Are All-on-4 Dental Implants?
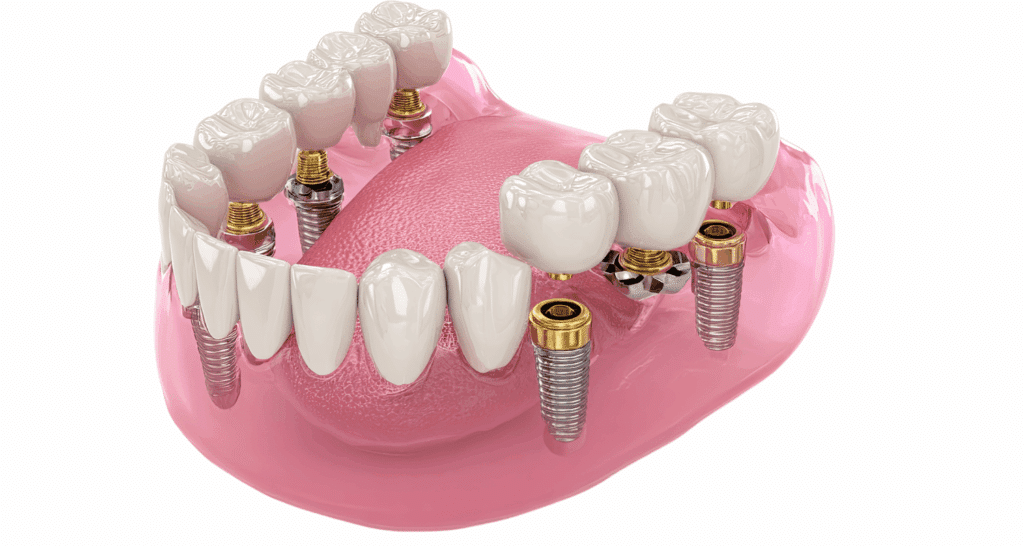
All-on-4 is a full-arch tooth replacement system. Four titanium implants are placed into the jawbone at specific angles to support a complete set of artificial teeth. The result is a fixed, non-removable set of teeth that looks and functions much like natural ones.
The procedure is popular because it requires fewer implants than traditional full-mouth restoration, often costs less, and in some cases allows patients to leave the dental office with temporary teeth the same day.
However, the success of All-on-4 depends heavily on the skill of the provider, the health of the patient, and the quality of aftercare. When any of these factors fall short, problems can follow.
Most Common Problems With All-on-4 Dental Implants
Implant Failure
This is the most serious risk. Implant failure happens when the titanium post does not fuse properly with the jawbone, a process called osseointegration. Without this bond, the implant becomes unstable.
Signs of implant failure include pain around the implant site, swelling in the gums, a loose or shifting prosthesis, and infection. Failure can happen in the weeks after surgery or years later.
The overall failure rate for dental implants is generally around 5 to 10 percent, and this risk goes up with poor health habits, smoking, or inadequate bone density. When one of the four implants fails, it puts more stress on the remaining three and may require the entire bridge to be remade.
Peri-Implantitis (Gum Infection Around the Implant)
Peri-implantitis is a gum infection that develops around the implant. It causes inflammation, bone loss, and if left untreated, can lead to implant failure. It is similar to gum disease but occurs specifically around implant sites.
Signs include bad taste or breath, bleeding around the implant, pain, swelling, and in severe cases, pus discharge or fever.
The biggest risk factors are poor oral hygiene and smoking. Bacteria that caused your original gum disease can return and damage the implants in the same way they destroyed your natural teeth.
If you have a history of gum disease, treating it before getting implants is essential. Periodontal therapy at Dental Faith can help get your gum health in order before any implant procedure.
Prosthesis Breakage or Wear
The bridge attached to your implants is not indestructible. Acrylic bridges, sometimes called hybrid restorations, are particularly prone to cracking and wear. The plastic teeth can chip or fracture off within just a few years.
Zirconia bridges are more durable, but even these can fracture if the bridge thickness is insufficient or if the patient grinds their teeth. Screw loosening is another common issue. The small screws holding the bridge to the implants can loosen over time, especially if bite forces are uneven.
Patients who grind their teeth at night carry a higher risk of breaking their bridge. A night guard is often recommended to protect the investment.
Bone Loss and Gum Recession
After All-on-4 surgery, some patients experience bone loss or gum recession around the implant sites. When gums pull back, the metal components of the implant or abutment can become visible. This creates both an aesthetic problem and a structural one.
Patients with naturally thin gum tissue are at higher risk. Some require a gum graft taken from the roof of the mouth before or after implant placement to prevent or address this problem.
Maintaining bone and gum health around implants requires consistent oral hygiene and regular dental checkups. Skipping these makes the problem much harder to catch early.
Bite Problems and Misalignment
If implants are not placed at the correct position or angle, the bite can feel off. Uneven bite pressure leads to jaw pain, clicking sensations, and accelerated wear on the prosthesis. In some cases, the bridge may need to be remade entirely.
This is one of the strongest arguments for choosing an experienced implant provider with advanced planning technology. Proper 3D imaging and digital treatment planning greatly reduce the risk of alignment errors.
Speech Changes
Because the All-on-4 bridge is a single fixed structure, some patients find it feels bulkier than natural teeth, at least initially. This can temporarily affect pronunciation, causing a slight lisp or change in speech patterns.
For most patients, this resolves within a few weeks as the mouth adapts. In rare cases, a speech therapist may help. Using digital pre-planning tools and testing prototype teeth before surgery can minimize this issue.
Food Trapping and Cleaning Difficulty
Traditional teeth are individual. All-on-4 gives you a connected bridge, which means there is a gap between the bridge and your gum line where food can collect. Cleaning under and around the bridge requires more effort than brushing regular teeth.
Patients who do not maintain proper cleaning routines under the bridge face a much higher risk of infection. Special tools like water flossers and interdental brushes are often necessary as part of daily oral care.
Surgical Risks
Like any surgical procedure, All-on-4 carries standard surgical risks including infection, bleeding, and reactions to anesthesia. Two more specific risks include:
Nerve damage: If an implant is placed too close to a nerve in the lower jaw, it can cause numbness, tingling, or ongoing pain in the lip, chin, or tongue. In most cases this is temporary, but in rare situations it can be permanent.
Sinus complications: When implants are placed in the upper jaw, there is a risk that they may extend into the sinus cavity, causing sinus inflammation or chronic congestion. This is more common in patients with low bone density in the upper jaw. Procedures like bone grafting or a sinus lift before implant placement can prevent this.
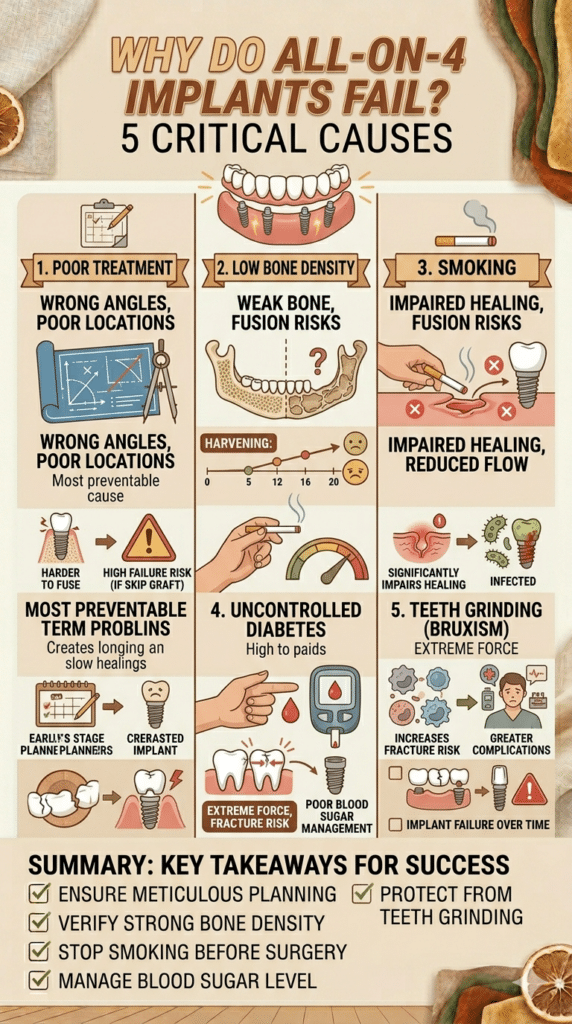
Why Do All-on-4 Implants Fail?
Understanding the causes of failure helps you make better decisions before and after treatment.
Poor treatment planning is one of the most preventable causes. Implants placed at wrong angles or in poor bone locations create long-term problems.
Low bone density makes it harder for implants to fuse with the jaw. Patients who need bone grafting and skip it face a much higher failure risk.
Smoking significantly impairs healing and reduces blood flow to the surgical site. Smokers have a much higher rate of implant failure and infection.
Uncontrolled diabetes affects the body’s ability to heal and fight infection. Patients with poorly managed blood sugar face greater complications.
Teeth grinding (bruxism) puts extreme force on the implants and bridge, increasing the risk of fracture and implant failure over time.
Real Patient Concerns and Regrets
Beyond the clinical risks, some patients report feeling disappointed with results that did not meet their expectations. Common concerns include:
The bridge feels bulky. Because the prosthesis replaces not just teeth but also missing bone and gum tissue, it naturally feels different from natural teeth. Most patients adjust, but some never feel fully comfortable.
The cost exceeded expectations. All-on-4 is a major financial investment, often ranging from $15,000 to $30,000 or more per arch. When complications arise and additional procedures are needed, costs climb further.
Maintenance is harder than expected. Many patients underestimate how much work goes into keeping the bridge clean and attending regular follow-up visits.
The teeth do not look natural enough. Aesthetic outcomes depend heavily on the skill of the dental lab and the dentist. Poor communication about expectations before treatment is a common cause of dissatisfaction.
How to Reduce the Risks
Most All-on-4 complications are preventable with the right approach.
Choose an experienced provider. Ask your dentist how many full-arch implant cases they have completed and for how many years. More experience generally means better outcomes.
Get proper imaging. 3D scans before surgery allow for precise implant placement and reduce the risk of nerve damage, sinus problems, and bite errors.
Commit to oral hygiene. Brushing twice daily, using a water flosser, and cleaning under the bridge every day is non-negotiable. Regular dental cleanings and professional monitoring are equally important.
Stop smoking before surgery. If you smoke, quitting before the procedure gives your implants the best chance to heal and fuse properly.
Use a night guard. If you grind your teeth, a custom night guard protects the bridge from excessive force and reduces fracture risk.
Attend all follow-up visits. Problems caught early are much easier and cheaper to fix. Skipping checkups allows small issues to become major ones.
Who Should NOT Get All-on-4 Implants?
All-on-4 is not right for everyone. You may need to wait or consider alternatives if you have:
- Severe bone loss that cannot be corrected with grafting
- Active, uncontrolled gum disease
- Uncontrolled diabetes or other chronic conditions affecting healing
- A heavy smoking habit you are unwilling to stop
- Poor oral hygiene habits you are unable to change
Exploring all your options is always a good idea. Dental implants and partial denture options may serve some patients better depending on their situation.
Pros and Cons of All-on-4 Implants
| Pros | Cons |
| Fixed, non-removable solution | High upfront cost |
| Improved chewing and speech | Surgical procedure required |
| Natural appearance | Healing time of several months |
| Prevents jawbone loss | Risk of implant failure |
| Fewer implants than traditional full-mouth restoration | Maintenance requires special tools |
| Long-lasting when well cared for | Prosthesis can crack or wear |
Are All-on-4 Implants Worth It?
For the right candidate, yes. Patients who are in good health, have adequate bone density, maintain strong oral hygiene, and work with an experienced provider tend to do very well. The improvement in quality of life, confidence, and daily function is significant.
But this is not a decision to rush. The procedure is surgical, expensive, and requires a long-term commitment to maintenance.
According to the American Academy of Implant Dentistry, dental implants have a very high success rate when performed by qualified providers and cared for properly. The key word is qualified.
At Dental Faith in Nashville, we believe every patient deserves a full, honest conversation about treatment options before making a decision this significant. If you are considering All-on-4 or want to know if you are a good candidate, a dental consultation is the right first step.
Frequently Asked Questions
What is the failure rate of All-on-4 implants?
Overall implant failure rates are generally between 5 and 10 percent. Risk increases with smoking, uncontrolled health conditions, and poor oral hygiene.
Do All-on-4 implants feel natural?
Most patients adapt within a few weeks. The bridge may feel slightly bulky at first since it replaces teeth, gum tissue, and bone. Over time, most people report it feels comfortable and natural.
What are the long-term problems with All-on-4?
Long-term issues can include peri-implantitis, bone loss, bridge fracture, gum recession, and screw loosening. Most of these are manageable with proper care and regular checkups.
Can All-on-4 implants be removed or replaced?
The bridge can be removed by a dentist for repairs or replacement. The implants themselves are fused to the bone and are much harder to remove. Revision procedures are possible but complex and costly.
Is All-on-4 better than traditional implants?
It depends on the patient. All-on-4 uses fewer implants and is often faster and less expensive than placing individual implants for every missing tooth. For patients with significant bone loss, it can also be a better fit. A consultation with your dentist will clarify which option suits your specific situation.
